“I have enlarged lacrimal glands. A biopsy was done on a lesion from one of the glands showing IgG:IgG4 ratio ~100% and 236 IgG4 blood level. I haven’t been officially diagnosed with IgG4-RD. What can happen if I refuse the prednisone?”
As part of our “Good Question” series, we address the following question from Angela:
“I have enlarged lacrimal glands. A biopsy was done on a lesion from one of the glands showing IgG:IgG4 ratio ~100% and 236 IgG4 blood level. I haven’t been officially diagnosed with IgG4-RD. I am lucky that I am only dealing with fatigue, difficulty falling asleep, puffy eyes, and arm pain now and again. What can happen if I refuse the prednisone?”
Dear Angela,
Thank you for reaching out with this question. This is a scenario frequently encountered in IgG4-RD and there is a very good chance that this is the correct diagnosis in your case. Similar findings can occur in other diagnoses, too, however, and it’s important that those also be considered.
The lacrimal glands are normally small organs that lie over the upper outer quadrant of each eye. Their purpose is to make tears to help keep the eyes moist and healthy. The combination of lacrimal gland enlargement (or "dacryoadenitis" in medical speak) with the substantial serum IgG4 elevation and the strongly suggestive biopsy findings make a strong case for a diagnosis of IgG4-RD. The three pictures show examples of lacrimal gland enlargement in IgG4-RD. Some cases of lacrimal gland enlargement in IgG4-RD are highly symptomatic, but most are not.
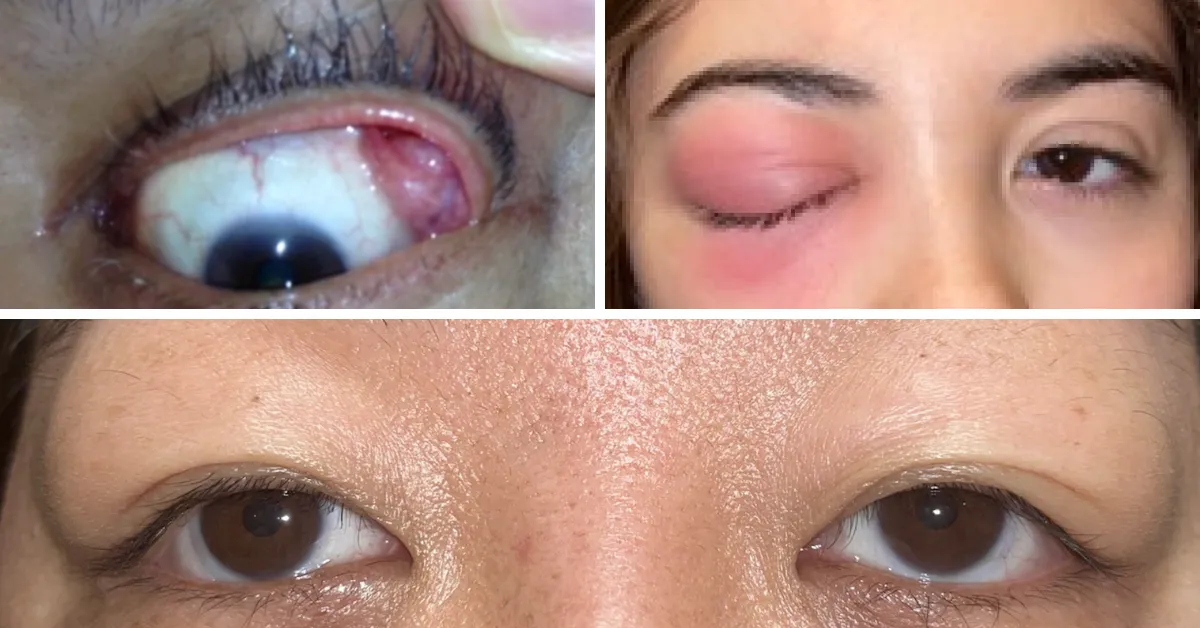
Examples of lacrimal gland enlargement in IgG4-RD.
Other conditions may cause this combination of findings though, so it is important that your doctors consider diagnoses such as granulomatosis with polyangiitis (GPA), sarcoidosis, and Sjögren's syndrome, among others. These other pictures (below) show examples of lacrimal gland enlargement in GPA (two pictures) and Sjögren’s syndrome (one picture), respectively. You can see why it’s important to differentiate these different diagnoses with further testing: they can look exactly alike. The testing is easy to do, however, and important, since the treatments for these conditions are quite different.
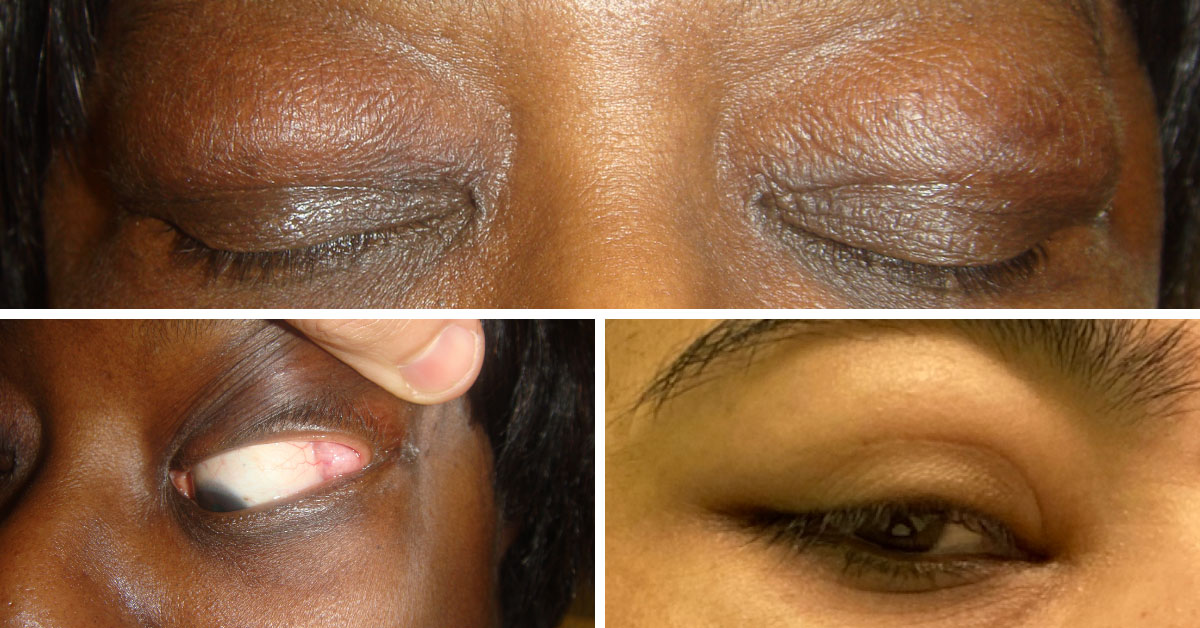
The top and bottom left photos show lacrimal gland enlargement in GPA. The bottom right photo shows lacrimal gland enlargement in Sjögren’s syndrome.
Ruling out these other conditions would involve several additional types of tests:
Blood tests. The performance of some additional blood tests, such antineutrophil cytoplasmic antibodies (ANCA) to help exclude GPA and anti-Ro antibodies to help exclude Sjögren’s syndrome.
Imaging. Imaging, particularly a CT scan of the chest and abdomen, and perhaps also the head and neck, to exclude disease (caused by either IgG4-RD or another diagnosis) in other parts of the body.
Careful review of pathology. Scrutiny of the available pathology – the lacrimal gland biopsy that you’ve already had – to make sure there are no tell-tale findings of other diagnoses. As examples, the finding of “necrosis” or intensive infiltration of neutrophils (white blood cells) in the tissue might suggest GPA, and the finding of well-formed “granulomas” in the tissue might imply that the diagnosis is sarcoidosis.
Your physicians have likely considered all of those things.
Assuming that the diagnosis is IgG4-RD, then the question is if and how to treat it. There are several points to consider in making this decision:
If the disease is confined only to the lacrimal glands, watchful waiting MIGHT be appropriate. Inflammation in the lacrimal glands that is not treated can often lead to severe dry eyes (after all, the lacrimal glands are the site of tear production). This can pose a significant impairment to quality of life and is well worth avoiding. The other symptoms that you have (fatigue, puffy eyes, etc.) are also most likely to worsen over time. Nevertheless, the need for treatment if indeed the only site of disease is the lacrimal glands is not urgent, and taking a “wait and see” approach might be reasonable for at least a while.
Having said that, most patients in this scenario eventually require treatment sooner or later.
If a “watch and wait” approach is adopted, then it is truly important to WATCH carefully, with a regular program of monitoring. This means regular follow-up appointments (every 3-6 months), regular blood tests (3-4 months), and perhaps follow-up imaging to make sure the disease is not getting worse or causing problems in other areas. IgG4-RD can sneak up slowly in other organs and it’s important to detect this early.
The additional testing, particularly the imaging, may be especially helpful in making a treatment decision now. The detection of IgG4-RD in other organs may have important implications, indicating that treatment now is really the best approach. Additional imaging could possibly reveal emerging issues in the pancreas, kidneys, lungs, lymph nodes, retroperitoneum, and so on. These would be crucial to identify and address, probably very soon.
We hope this is helpful, Angela. You’ve probably discovered that the Foundation website provides a lot more information about IgG4-RD (please see Resources), its specific organ manifestations, and approaches to treatment. Thank you for sharing your story.
Stay up to date with IgG4ward!'s weekly "Good Question" by joining the IgG4ward! Online Community.




